We realize it has been a while since we last posted. Life has just been so terribly busy lately. Here’s the rundown of what’s been happening.

Hazel has been recovering nicely since her PDA surgery. She had some ups and downs on her oxygen needs at first. A follow-up ultrasound of her heart shows no issues with the closure they did on her ductus, and blood is all flowing in the proper direction. Since then she has been stable enough that we have both been fortunate enough to do some kangaroo care with her during this time.
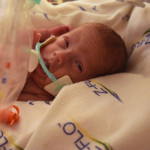
Grant has had a few more milestones. His oxygen needs were pretty high, in the 70% range. At some point, the care team decided that he was trying enough breaths and it might be worth trying to move him from the high frequency oscillating ventilator to the conventional ventilator like Hazel is on. Grant handled it magnificently and we were able to hold him again! Grant had not been held in over six weeks! The high frequency ventilators have a really stiff tube that makes it too difficult to hold the babies while they are on them. We were glad to take advantage of the chance to hold him. He has grown so much since we last held him, it was like holding a completely different baby.

At this point, both kids have at least doubled their weight since birth. Grant weighs 3 pounds, 5 ounces and Hazel weighs 2 pounds, 5 ounces. The weights shift a bit from day to day, as transfusions, blood draws, feedings, medications and infections can all affect the fluid they retain and obscure their real weight gains from growth.
Not long after Grant switched ventilators, he was having challenges with getting all the air he needs from the vent. As the babies grow, the space between their windpipe and the endotracheal tube (ET tube) gets bigger and causes air to leak. Grant’s leak was getting big to the point where they were fighting just to keep his lungs inflated against all the air loss. One option is to put in a larger ET tube, but the other is to try to move him off the ventilator to a CPAP or SIPAP. In case you aren’t familiar with either, a CPAP creates a constant air pressure and a SIPAP creates waves of higher pressure much like breaths, neither of which needs a breathing tube but instead connect to the nose with a headgear. In either case, the baby is doing the breathing with just a little aid of pressure to keep the lungs expanded.
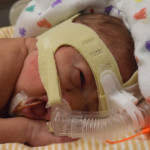
Well, the care team made the choice to move him to the SIPAP and so far (he has only been on the machine for a few hours) he has been doing great and his blood gas labs show he is getting respectable numbers. We have been told that most kids fail their first time eventually, but every minute and hour helps to train the breathing and develop their lungs. We’re hopeful he will do very well, even if he does have to step back to a ventilator, and we are totally thrilled to see this progress. The best part is, for the first time ever, we were able to hear Grant cry! We never thought we would want to hear a baby cry and be happy with it, but it was such a wonderful sound.
A few weeks ago, they discovered a fungus in one of Grant’s blood cultures and started an antifungal treatment. He has not had a positive culture since the initial finding and will be finishing his antifungal treatment tomorrow, which means his PICC line (peripherally inserted central catheter) can be removed after that. The PICC lines are a convenient way to administer medication and fluids, but they are also prone to infection, so it is a good thing to have removed when possible.
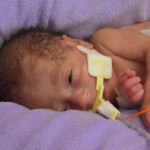
We are looking forward to further progress for both. Hazel is probably not far behind, but her nose is still just too tiny for the mask and they want her to be bigger and stronger before they make the CPAP/SIPAP transition for her.
We feel so very fortunate with all the progress the babies have made. We know they still have a long path ahead of them, and their outcomes are yet to be determined in the long term. For now we are living in the moment and are so proud of Hazel and Grant and will enjoy holding them and watching them grow!
