
I feel like I don’t know where to start with this post. Since our kids were born, I’ve lost all sense of time. Little things like getting a meal seem to take forever, and an hour in the NICU goes by in the blink of an eye. People are asking for updates, and I feel bad that we haven’t had time to post any updates through the blog. Here are the basics:
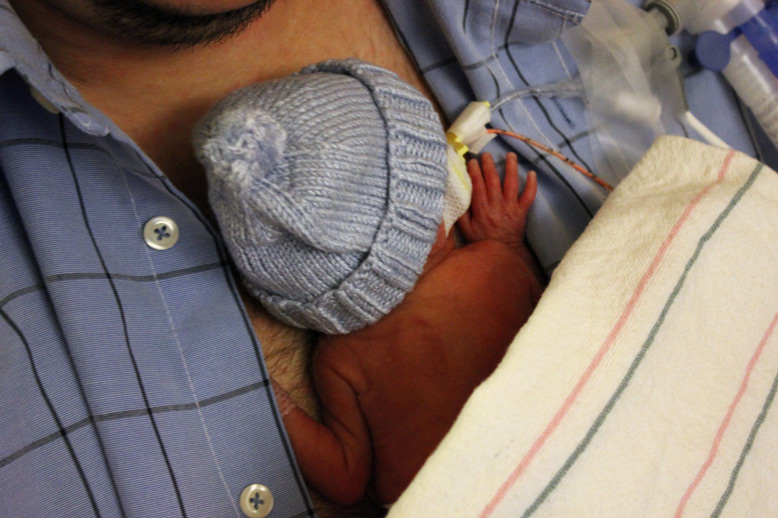
Hazel and Grant continue to fight for their lives daily. They were born at the edge of viability and the doctors have warned us that their stay in the NICU will be full of ups and downs. Bodily systems we normally take for granted are monitored daily for changes. Breathing, blood pressure, heart rate, hemoglobin, platelets, feeding, urine and stool are daily subjects for updates we get from the NICU team. We are learning a lot about the struggle typical of preemies and amazed at their fragility and endurance. We have both had the chance to hold Grant outside of the incubator, but Hazel has not yet been stable enough for this.
Infections are always a big concern. We wash our hands thoroughly and use hand sanitizer before we can touch or hold our babies. Even with all these precautions, it is not a completely sterile environment. The tubes and lines going into their bodies will need to be changed periodically, either because of risk of infection or an actual detected bacteria formation.
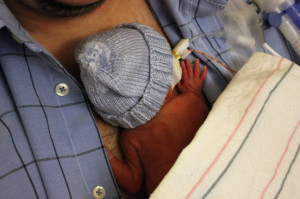
For their privacy, I won’t go into details about particular daily challenges each faces on this blog. Everything is in constant flux, so by the time you read it, the situation may have changed. There may have been changes from the last NICU update by the time I write this. We will share more information in private conversation, but we’ll limit sharing with the internet.
Julie has been through a lot in the past week and a half. I continue to be amazed by her. She went in expecting a long stay in the hospital as we awaited the arrival of the triplets. She dreaded the loneliness, boredom and homesickness, but was willing to go through it for the kids. In less than a week, she started having contractions. At first she thought they were just the babies moving, but the monitors were detecting otherwise. Within about an hour of the first signs of contractions, they started to become painful for her and she was placed on magnesium sulfate, which is used primarily as neural protection for the babies in case they would be born but it can also have the effect of stalling contractions. Overnight the contractions continued, and we were moved from her antepartum care room to the labor and delivery area “as a precaution.”
The day’s contractions became increasingly painful, and Julie was given an epidural for the pain. She went through painful examinations of her cervix and ultrasounds. In the last ultrasound, the doctor had trouble seeing Baby A, and did a manual examination in which he discovered she was already starting to emerge. Julie was rushed into the operating room, where she delivered Marissa Jean vaginally. I saw Marissa’s hand move before she was quickly picked up by a nurse. We were in great suspense as the NICU team worked on Marissa in an adjacent room. At this time Julie was getting a cerclage (had her cervix stitched shut) to help keep the other two babies in and give them hope at a longer term in the womb. The NICU doctor returned to inform us that despite their best efforts, Marissa’s lungs were just not developed enough to get air into them. She was wrapped in a blanket and brought into us. We held her and sobbed. A doctor or nurse returned a few times to check her heartbeat until it could no longer be detected.
That night we were surrounded by close family as we mourned our loss. She was already missed as a daughter/granddaughter/niece.
Our hope turned to the other two babies, thinking that perhaps they would be able to make it in the womb for a couple more months. They still had their amniotic sacs, after all. The contractions were starting to subside, and Julie could now be on medication to prevent contractions and labor. In spite of all our hopes, the contractions returned. Julie was again moved to Labor and Delivery for closer monitoring.
This time, the contractions started placing increased stress on Baby B. Each contraction lowered the heart rate significantly, to the point that it was scary to watch the rate drop and the heartbeat would be barely audible through the monitor’s speaker. After a while of this, the doctors made the decision to do a c-section delivery of the other two babies.
Julie was prepped and wheeled away. I was told they would come get me in ten minutes. Ten minutes in hospital speak means “just keep waiting.” They finally led me into the operating room where it seemed the procedure was well under way. Julie had a spinal but was still extremely tense and uncomfortable. I can’t imagine what she was going through. Because of the surgical dressing, I couldn’t see anything, but I could hold the camera out enough to record the nurses who were ready to collect the babies as they were born.
“BIRTH!” they shouted out, followed by “thirty-six” – designating the time of birth. A baby flew by so quickly I couldn’t really see much. About 40 seconds later I heard the same declaration and time, followed by another baby being transported just as rapidly. I was left to simply comfort Julie as they proceeded to remove the three placentas, stitch her up and remove the cerclage stitches.
Someone placed bracelets on our wrists. I knew this was a good sign and reassured Julie, but she was still very stressed by everything she was going through at the moment.
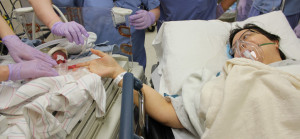
The doctor came to get me and introduce me to my son, then to my daughter, neither of which yet had a name. Each were in their “Giraffe” beds and hooked up to breathing tubes and wrapped in plastic bags to retain heat. Our boy was carted away and Julie was wheeled into the room on her bed to meet our daughter. It was a very touching moment as she laid eyes on her for the first time and was able to hold her hand. I did my best to get both photos and video of the moment. Julie was then carted away to her room and I followed the NICU team to our kids’ room. I don’t even remember this trip, and I only know because I have the photos from when they first arrived in the room and can recall making the decision to go check on Julie at one point.
Julie was still extremely tense and agitated from everything. I think she found the will to overcome all the pain medications they administered, and I was there to witness everything she received. I did my best to calm her, talking her through breathing and positive imagery until she finally settled down. I then went back to Julie’s antepartum care room where immediate family was waiting so I could quickly share the news before going back to Julie.
After a while, Julie’s bed was rolled to the NICU so she could finally see Grant and see Hazel again. Then we returned to her antepartum room, completely wiped out. Over the last 76 hours, Julie had been in labor with contractions, received six IV pokes, got liters of drugs and fluid, delivered both vaginally and by c-section, received a cerclage, had a cerclage removed, named three kids and lost a daughter. She did all this with very little sleep. This was not the end, as she developed a fever, likely the result of an infection.
Julie was discharged on a Wednesday, and I had made plans to pick her up. We were both having such a difficult time in our grief. Julie was not ready to be separated from the kids, and I didn’t want to leave any of them there. I had already had difficulty being at work for only a day and a half that week. The hospital offered to let us stay in the room as it was not immediately needed, and we accepted the gracious offer. We finally went home that Saturday, after both kids had a “good” day in the NICU.
We are very thankful for everyone’s thoughts and prayers. Our entire family will need these for some time.
Many many continued prayers for your beautiful family and you are in my thoughts everyday.